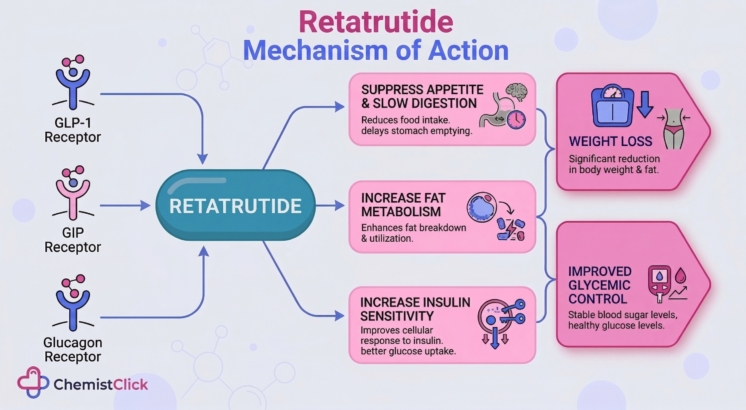
Retatrutide works by activating receptors for GLP-1, GIP and glucagon.
These are natural hormones involved in appetite, digestion, blood sugar and energy balance.
Retatrutide is described as a triple hormone receptor agonist, and informally referred to as “triple-G”.
The 3 hormones retatrutide acts on:
GLP-1: helps you feel fuller and eat less
GLP-1 is a natural gut hormone released after eating. It helps reduce appetite, slows down how quickly food leaves your stomach, and helps you feel full for longer.
This is why medicines that act on GLP-1 can help people eat less without feeling as hungry all the time.
GIP: helps your body respond to food, supporting weight loss
GIP is another hormone your body releases after food. It helps your body release insulin when needed and may work alongside GLP-1 to improve blood sugar control and appetite regulation.
Better insulin control results in fewer blood sugar spikes and crashes, which can help to reduce hunger and cravings. Your body is less likely to stay in a cycle of overeating driven by poor blood sugar control
Glucagon: can help the body burn more energy
Glucagon usually helps raise blood sugar when it drops too low, but it also seems to affect how the body uses energy and fat.
In retatrutide, glucagon activity appears to help the body use more energy, which means the body can burn more calories. This is one of the main reasons experts are interested in retatrutide, because it does more than just reducing appetite.